AllForms vs Assured
Side-by-side comparison to help you choose the right product.
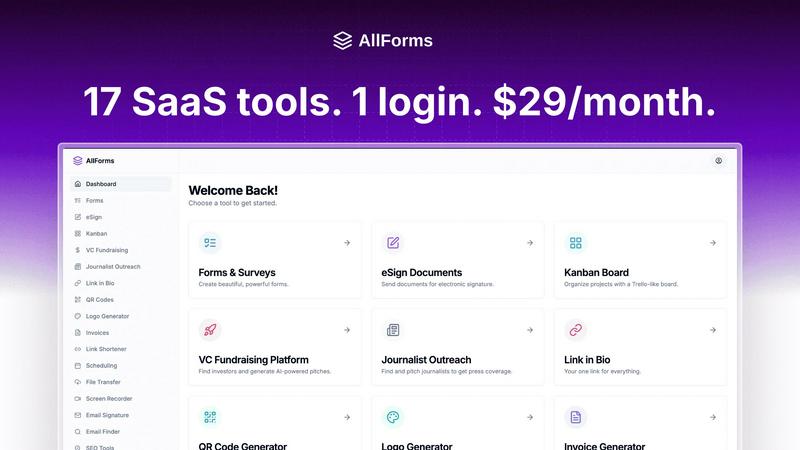
Unite your team with 17 essential tools in one seamless, affordable platform.
Last updated: March 1, 2026
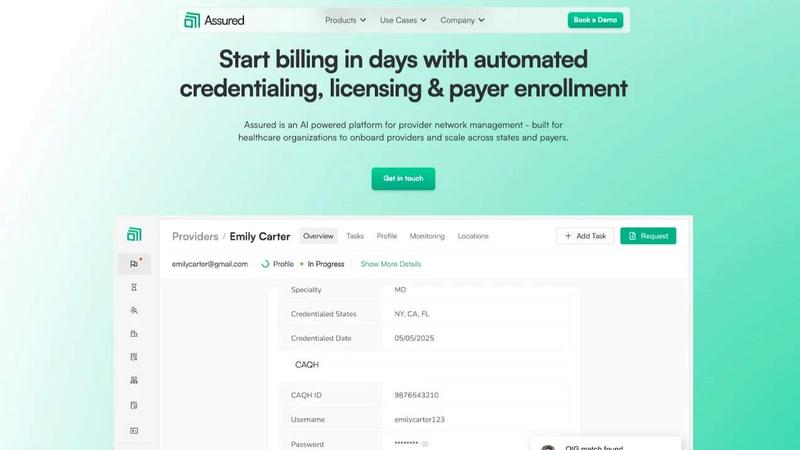
Assured
Assured uses AI to automate provider credentialing and enrollment so healthcare companies can start billing in days, not months.
Visual Comparison
AllForms
Assured
Overview
About AllForms
AllForms is the ultimate collaborative platform designed to unify your team's essential tools and eliminate the friction of disconnected workflows. It's a revolutionary all-in-one SaaS solution that consolidates the core functionalities of 17+ expensive, standalone applications into a single, seamless, and beautiful interface. Built for modern businesses and forward-thinking teams, AllForms empowers professionals across sales, marketing, operations, and leadership to work together more effectively by breaking down software silos. Its core value proposition is profound synergy: by replacing a costly patchwork of subscriptions—from e-signing and scheduling to AI chat and SEO tools—teams can achieve unparalleled operational harmony. This consolidation not only drives massive cost savings, exceeding $14,000 annually, but also enhances collective productivity, ensures data continuity, and simplifies management. AllForms is tailored for any team tired of juggling multiple logins, exporting/importing data, and suffering from clunky, slow tools. It fosters a cooperative environment where every function, from client contracts to marketing outreach, is interconnected, allowing the entire organization to focus on shared goals and accelerated growth.
About Assured
Assured is an AI-powered provider network management platform built to help healthcare organizations scale efficiently and stop losing revenue to administrative delays. It automates the complex, manual processes of credentialing, licensing, payer enrollment, and ongoing network monitoring. Designed for provider groups, health systems, payers, and digital health companies, Assured tackles the core problem of disconnected data and slow, error-prone manual work. Its core value proposition is dramatic speed and accuracy: get providers credentialed in 48 hours instead of 60+ days, achieve 95% first-pass approval rates for payer enrollments, and detect sanctions 22 days earlier than manual methods. As an NCQA-certified Credentials Verification Organization (CVO), Assured leverages AI to verify credentials across 2,000+ primary sources in parallel, auto-generate applications, and submit directly to payer portals. This means faster provider onboarding, quicker revenue generation, and complete peace of mind with real-time data monitoring, all from a single, centralized platform.